Candida Auris: The Superfungus that could be Worse than COVID-19
The health systems of several countries are concerned about the health emergency that could be caused by Candida Auris, a superfungus resistant to antibiotics
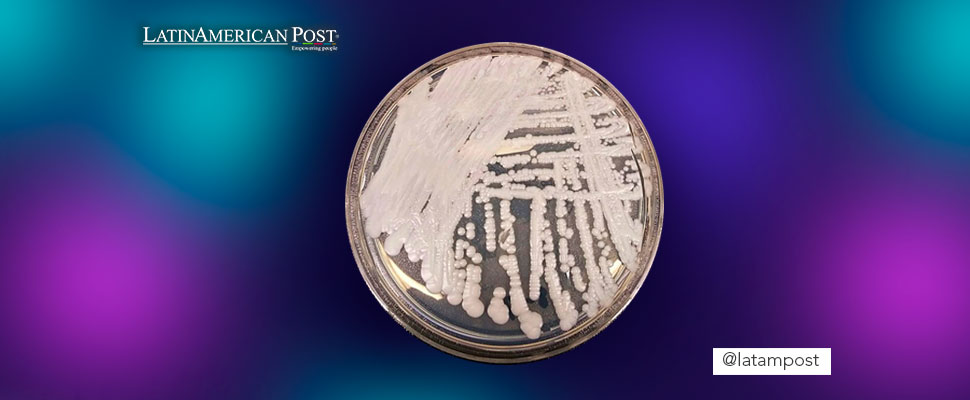
Photo: CDC
”
LatinAmerican Post | Brandon Martínez
Today the world is facing an enemy that could be worse than the coronavirus. It spreads silently in different regions of the planet, it is extremely deadly and it seems that it is immune to practically everything that tries to exterminate it.
It is “Candida Auris” a drug-resistant fungus that is already considered a global threat and that in the past has wreaked havoc in countries such as Venezuela, the United States, Spain and England.
This problem is described in the United States as an “urgent threat” because it is almost impossible to eradicate it, because it has a strong mechanism of resistance to all types of chemicals when it is installed on surfaces.
Where was the Superfungus originated?
The first case dates back to 2009 in Tokyo. A 70-year-old woman was hospitalized and this superfungus was found inside her ear. Different treatments were used to eliminate the infection in the patient, but all failed. However, microbiologists Kazuo Satoh and Koichi Makimura managed to isolate it and decided to call it “Auris” after the atrial space where it was found.
It is currently known as Candida Auris and is a yeast-type fungus. According to the US CDC, this agent is often highly invasive and usually resides in hospital facilities. However, it also manages to settle permanently in any place, which creates a serious risk for people.
For a few months, this infectious agent has been affecting people in the states of New York, New Jersey, and Illinois in the United States.
However, information from the Center for Disease Control and Prevention warns that people who contract it die before three months. On the other hand, it yields important data, such as the number of infected that as of March 29 of last year already totaled 587 confirmed cases in the North American country.
Lee también: ¿Sabes lo que es el Hongo Negro y cómo se contrae?
Likewise, Brazil has recently reported a local outbreak of Candida Auris, accounting for three infections. For its part, Colombia has added at least 17 cases of this microorganism since 2017. Of this last figure, a mortality rate of 35.2% was recorded in less than a month.
What makes it so dangerous and why is it a latent threat?
Candida Auris is a very dangerous external agent. It is a fungus that epidemiologists fear, because its spread is cautious and its effects are deadly.
This super fungus has developed an innate resistance in its evolution over approximately 4,000 years. However, this yeast has increased its adaptation mechanism thanks to the indiscriminate use of antibiotics in humans. This means that people have been consuming antibiotics unnecessarily or inappropriately, which has allowed these germs to become more cunning and become immune against current medicine. Becoming a headache for the scientific community.
Practically, the pathogen cannot be eliminated from the surfaces where it is installed. In addition, the new antibiotics produced by pharmaceutical companies have no effect on it. Therefore, it could be said that humanity is facing an unstoppable enemy.
What happens when someone gets infected with Candida Auris?
The superfungus mainly invades the blood. From there, it settles in different organs or systems such as the brain, kidneys, liver, bones, muscles, joints, spleen, and eyes. This is known as candidiasis.
This condition manages to weaken the entire human body, causing the patient to die in a short time. After this fact, there are people more vulnerable to the severity of the infection, for example, people with low defenses, cancer, diabetics and those who have used antibiotics repeatedly and irrationally.
How can it be avoided?
The only way to be free of Candida Auris is to maintain hygiene measures; like constant hand washing; use of gloves if fluids or blood are to be handled; facial protection if there is possible contact with contaminated elements; sterilization and cleaning of elements if there is suspicion of infected people in the environment. But, the most important thing is to avoid self-medication with antibiotics.




